 Photo: Getty
Photo: Getty Before you make big changes to your child’s diet or your own diet, it’s important to see an allergist for allergy testing to properly confirm a diagnosis.
“A good analysis will make a much more clear answer whether or not you have a food allergy,” says Dr. Marshall Plaut, who is chief of the food allergy, atopic dermatitis and allergic mechanisms section for the National Institute of Allergy and Infectious Diseases (NIAID).
Following is a guide to the different forms of food allergy tests, largely based on the most recent NIAID guidelines for food allergy and leading experts.
Physical Exam and Patient History
All forms of allergy testing, even when the results seem to be strong, must be considered together with a physical exam and a detailed patient history – both of which can help narrow down what food might be the trigger.
“You have to look at all the pieces of the puzzle because none of the tests by themselves are predictive enough of a diagnosis of a clinical allergy,” Plaut says.
The physical exam and patient history also provide important clues, such as symptoms that could indicate whether or not the allergy is mediated by IgE antibodies. These are important for determining which tests to get.
Skin-Prick Allergy Testing
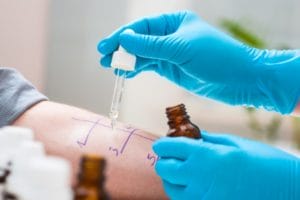 A skin prick allergy test. Photo: Getty
A skin prick allergy test. Photo: Getty Skin-prick testing (SPT) is the most common form of allergy test and is used to try and identify the specific foods that a patient may be allergic to. For this test, which is typically done at an allergist’s office, drops of different serums containing individual allergens will be put the on patient’s forearm or back. A medical professional will then use a small needle to prick the skin – this feels like a small poke with a pin – so that the serum goes beneath the skin.
Then it’s a waiting game. The patient’s skin may react by forming a reddish hive, or wheal, at specific prick spots, indicating that the IgE antibodies in the skin responded to the food allergen in that serum.
A test is considered “positive” for a particular allergen if the diameter of the hive is 3 millimeters or greater than a prick site made with no allergen (known as the negative control). The bigger the hive, the more likely it is that you will react if you eat that food.
However, a positive skin-prick test alone is not enough to confirm a food allergy, as false positives occur quite frequently (e.g. when a person has been eating a food with no symptoms but still tests positive). So the allergist will consider the skin test’s results in combination with the symptom history and physical exam. There are also some cases of false negative skin-prick test results. While uncommon, these may occur if an allergen extract is too diluted or antihistamines were not avoided prior to testing.
Blood Test (ImmunoCap, TurboMP, Immunite)
The blood test recommended by NIAID is the “allergen-specific serum IgE” test that looks at antibodies for specific food allergens (sIgE) in the blood. The blood test for specific allergens is an imprecise tool, so leading allergist organizations do not recommend blood tests in the absence of a history of symptoms that could be allergy-based. With such prior symptoms, the blood test can help to indicate the chance that a person is allergic to certain food or foods.
Often the allergist will do the blood test in addition to the skin-prick test to assist in diagnosis. The blood test is particularly useful if a skin-prick test cannot be done, for instance if the patient has severe eczema.
The higher the level of the specific IgE for a food allergen, the more likely that eating that food will result in an allergic reaction. However, as with skin-prick tests, these results only indicate a “possible” food allergy, and are not enough on their own for a diagnosis.
This is not a “yes or no” test like the results of a pregnancy test that show whether a woman is pregnant – or not. There are cases where patients with low specific IgE do have a food allergy based on their history or further assessment.
Component Testing
This relatively new form of IgE blood test looks at the specific proteins (or “components”) of an allergen that cause a reaction, rather than the allergen as a whole.
“There are a number of proteins within things like peanuts and tree nuts that cross-react with pollens,” Dr. Hugh Sampson, director of the Jaffe Food Allergy Institute at Mount Sinai in New York, noted at the 2017 AAAAI allergists’ meeting. This cross-reaction can throw off the results of the usual blood tests, making it appear as if a patient is highly reactive to peanuts or tree nuts, depending on the pollen season.
For a patient suspected to have a peanut allergy, component testing would look at the IgE antibody levels for different peanut proteins. If the patient has high levels for the Ara h 2, studies show that this is a good indicator that the person is peanut-allergic. However, if that person has high levels of Ara h 8 or 9, then the symptoms are likely to be linked to a cross-reaction with pollen, a less severe condition known as oral allergy syndrome.
“Component testing has come more into its own and it’s likely to become more useful, however, it’s still not 100 percent predictive,” says Plaut. “If you have IgE to Ara h 2, at this point you still need a clinical history and a physical to confirm the diagnosis.”
Atopy Patch Test
These tests are not recommended by NIAID for food allergy, since skin-prick tests give more accurate results. However, Plaut points out that patch tests can be useful for predicting other allergic conditions, such as those who have delayed reactions or a form of non-IgE mediated allergy.
Intradermal Allergy Testing
For this form of test, small amounts of a food allergen are injected directly into the skin. However, it carries a higher risk of severe reaction and has not been proven to be more effective compared to the skin-prick method. It is therefore not recommended by NIAID.
Oral Food Challenge
The oral food challenge is typically done after skin-prick tests, blood tests, or other tests. It is considered the “gold standard” of reliability to confirm an allergy diagnosis. Such a challenge is done under medical supervision, since a patient actually consumes a small amount of their suspected allergen.
Beforehand, patients may be asked to remove the suspect food from their diet for a few weeks. The test, typically conducted at an allergist’s office or a hospital if there is a higher risk of reaction, begins with the patient eating a low dose of the suspect food, less than what is expected to cause a reaction.
Over the course of several hours, the patient will continue to receive gradually increasing amounts of the suspect food, and be monitored for any signs of a reaction. If the patient is reaches the dose that is equal to a normal portion without reacting, the food is considered safe to eat. If a patient experiences a reaction, the challenge is stopped and the reaction is treated.
These tests can help confirm a food allergy and the type of food allergy based on the reaction that is observed, but as with all tests, must be considered in conjunction with a patient history and physical. See also: 5 Reasons Patients Shun Oral Food Challenges.
Food Tests to Avoid!
NIAID strongly recommends steering clear of the following allergy tests because they are unregulated and/or scientifically unproven to accurately indicate a food allergy.
Basophil histamine release/activation
Lymphocyte stimulation
Facial thermography
Gastric juice analysis
Endoscopic allergen provocation
Hair analysis
Applied kinesiology
Provocation neutralization
Allergen-specific IgG4
Cytotoxicity assays
Electrodermal test (Vega)
Mediator release assay





